Case Studies
The following case studies illustrate the effectiveness of NovoSorb® BTM. The studies are provided with consent from the patient and their surgeons. They are intended for educational use only. To view testimonials from patients whose lives have been changed by NovoSorb technology, see our Patient Stories
-
Trauma
-
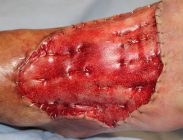
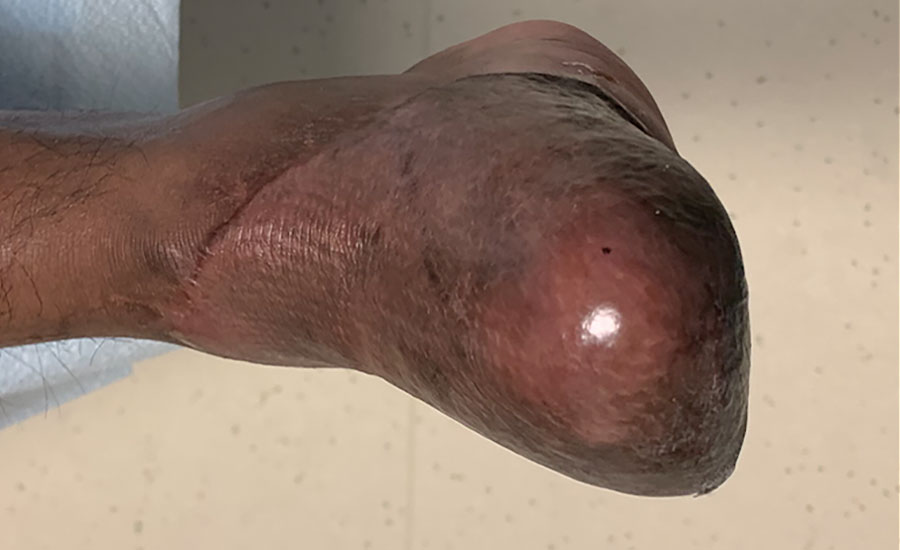
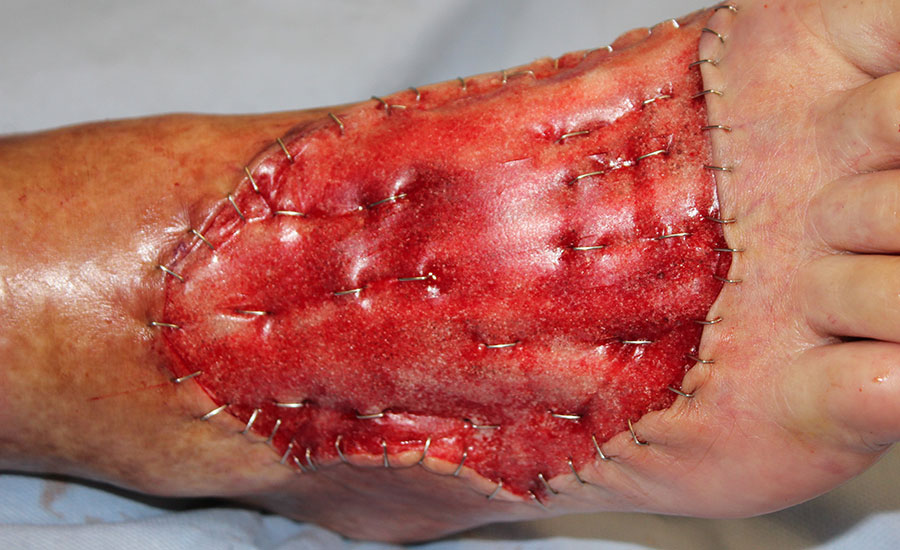
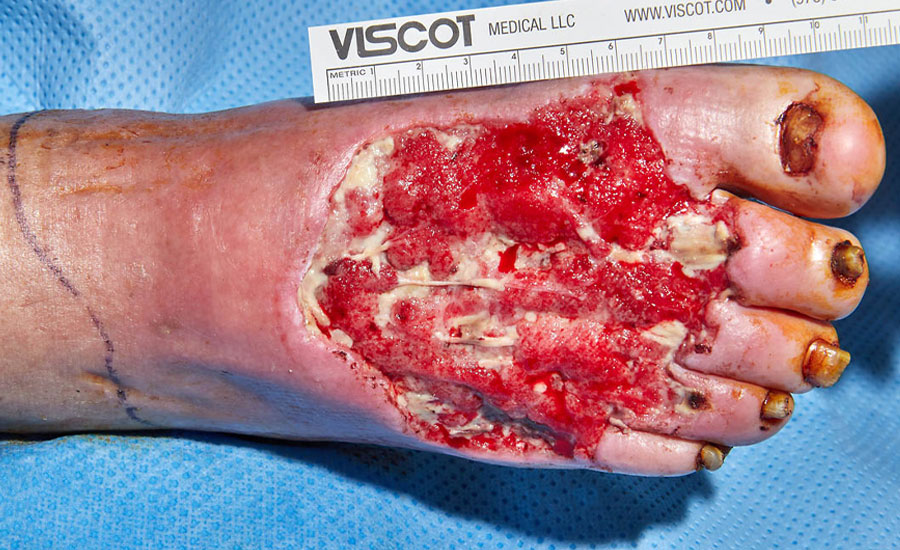
Patient’s right foot was pinned under a moving railroad car resulting in a severe crush injury. Injuries included full avulsion of all dorsal soft tissue, all 5 digits, and plantar aspect sparing the heel, as well as amputation of the 1st-5th distal phalanges. A below knee amputation (BKA) was initially recommended. Risks and benefts of BKA versus salvage were discussed and the decision was made to save the limb.
NovoSorb BTM was applied over exposed bone, tendon and muscle, secured with staples and dressed in NPWT. Patient was ambulatory on postoperative day (POD) 2. BTM showed signs of vascularization without infection at POD 17. At day 30, skin graft was applied with 100% graft take. The avoidance of an amputation greatly impacted the patient’s self-image and he is ambulatory with minimal usage of a cane.
-
Patient was involved in a traumatic motor vehicle roll-over injury with several open fractures/ dislocations on three fingers. Soft-tissue debridement of devitalized tissue was performed with NovoSorb BTM applied directly over exposed bone, joint, and tendon. BTM was applied initially as a Temporizing dressing until more complex reconstruction options could be explored. Early vascularization without infection led to a decision to follow patient clinically. At day 41 following delamination, the wounds spontaneously re-epithelialized before scheduled skin grafting. At the 3-month follow-up there was no tissue breakdown and the patient was able to avoid further reconstructive surgery.
-
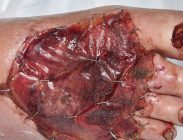
Patient sustained a traumatic degloving injury to their right foot. Soft-tissue debridement of the dorsum of the foot performed, with exposure of the deep structures. Free flap tissue surgery was deemed unacceptable to the patient due to associated risk and donor site morbidity.
NovoSorb BTM was applied after second-look debridement on Day 3 and regular dressing changes were performed twice weekly. At 9 weeks BTM was delaminated and split-thickness skin graft applied. Seven months after grafting the skin displayed excellent conformity, and range of motion was restored with no tethering of the underlying tendons.
-
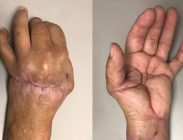
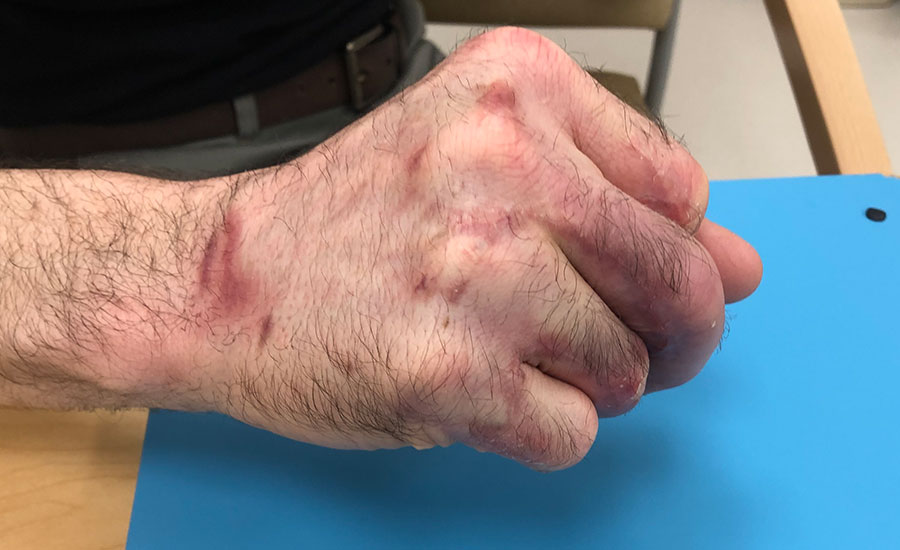
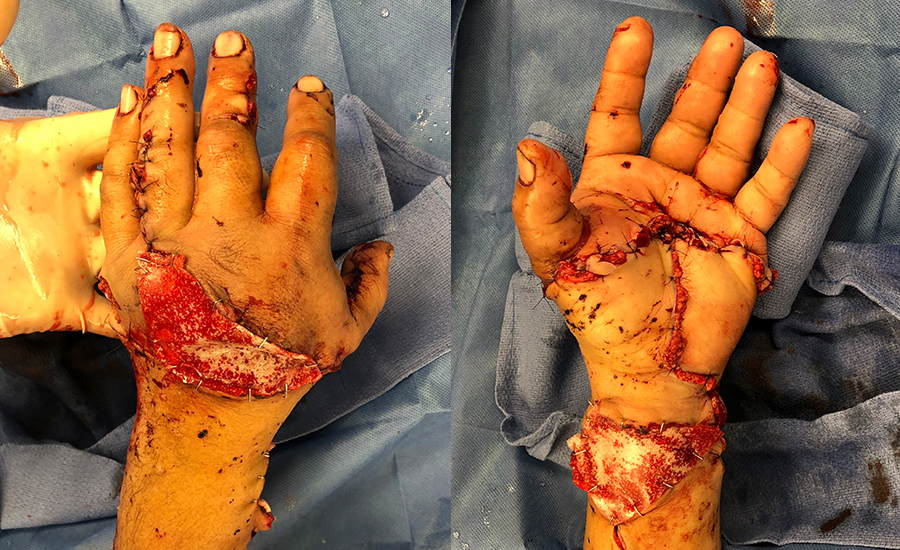
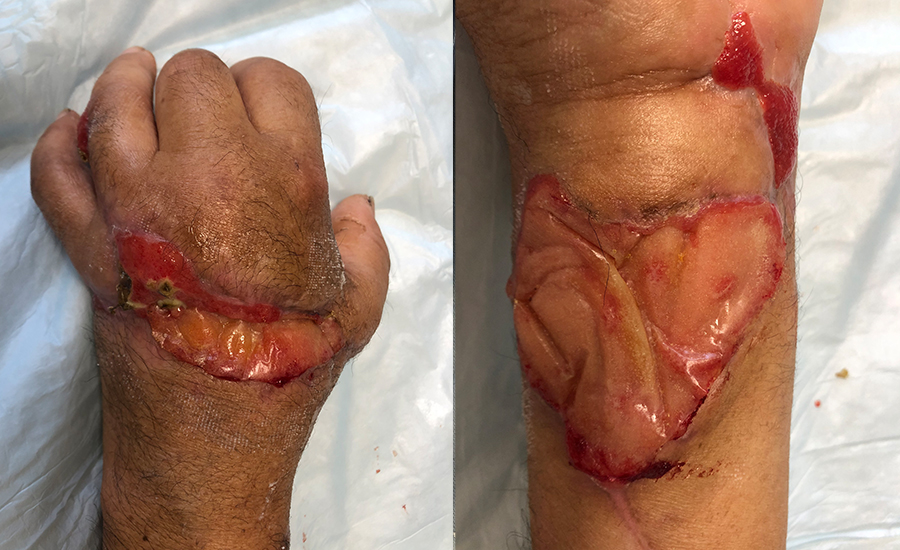
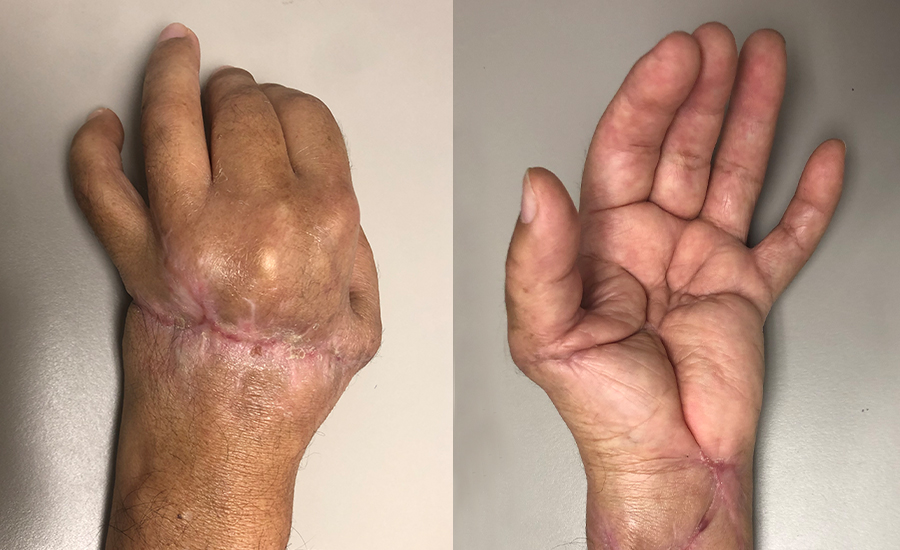
Patient sustained a transmetacarpal amputation of their left non-dominant hand and a forearm laceration while using a saw at work. A successful replantation was performed, and the patient was left with two defects: one to the dorsal hand and the other to the volar forearm. Due to edema, the defects could not be closed primarily. NovoSorb® BTM was chosen as an alternative over a more complex tissue flap reconstruction to offer immediate coverage and to minimize surgical time. For the dorsal wound, NovoSorb BTM was applied directly over the exposed extensor tendon and vein grafts; and, for the volar wound, over the median nerve and flexor tendons. Both wounds re-epithelialized without requiring skin grafting or additional revision surgery.
-
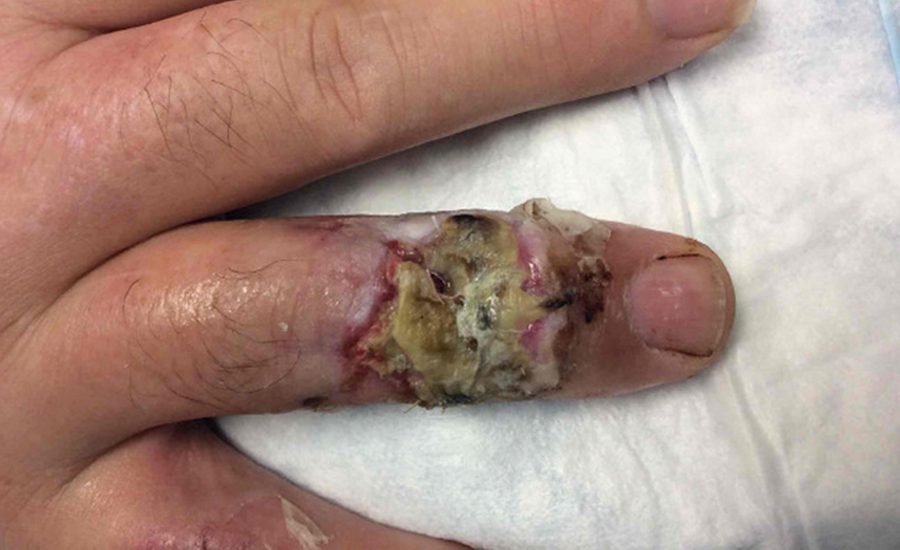
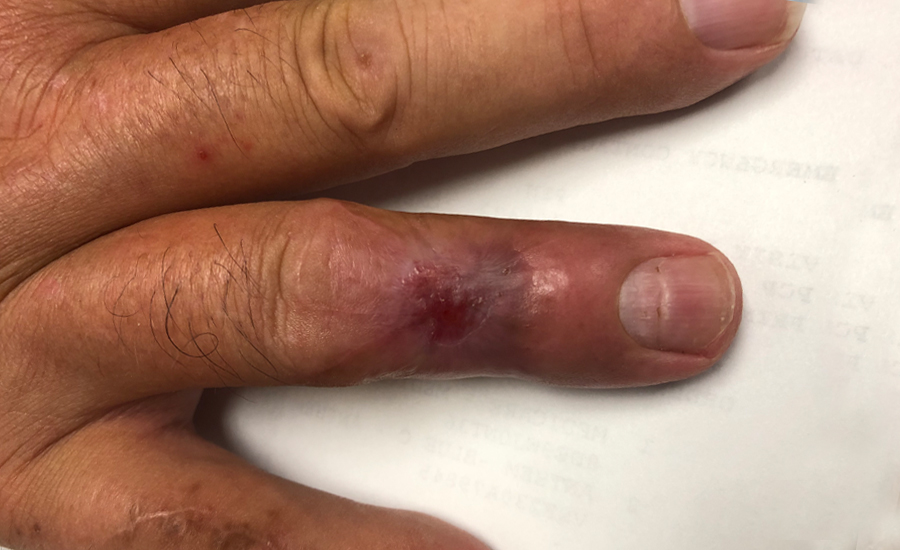
Patient sustained a self-inflicted gunshot wound to the ring finger resulting in a middle phalanx fracture and a dorsal soft-tissue defect. Initial soft-tissue reconstruction with a full-thickness skin graft over the fracture and extensor tendon repair was unsuccessful. To avoid further donor site morbidity and to maximize functionality, NovoSorb® BTM was chosen to salvage the finger over more complex local flap options. NovoSorb BTM successfully integrated over the exposed bone, which was devoid of periosteum. After the NovoSorb BTM sealing membrane was removed, the wound bed was left to re-epithelialize, eliminating the requirement for a skin graft.
-
-
Infectious Diseases
-
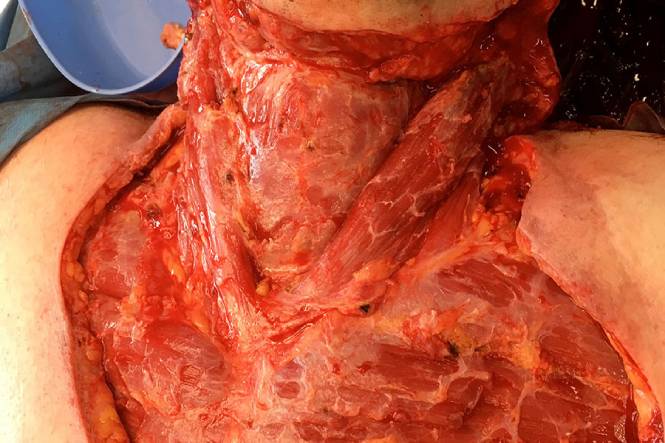
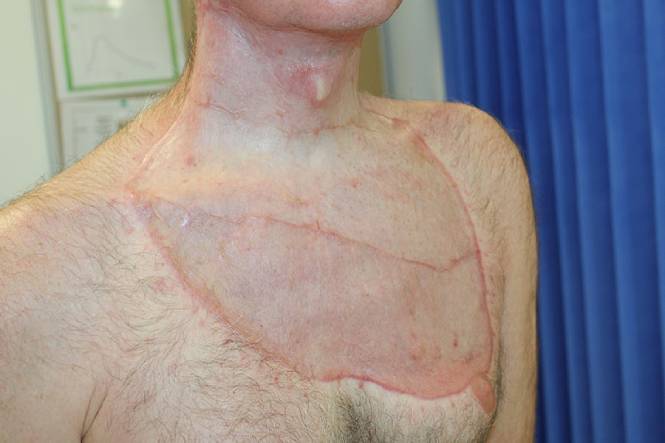
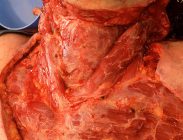
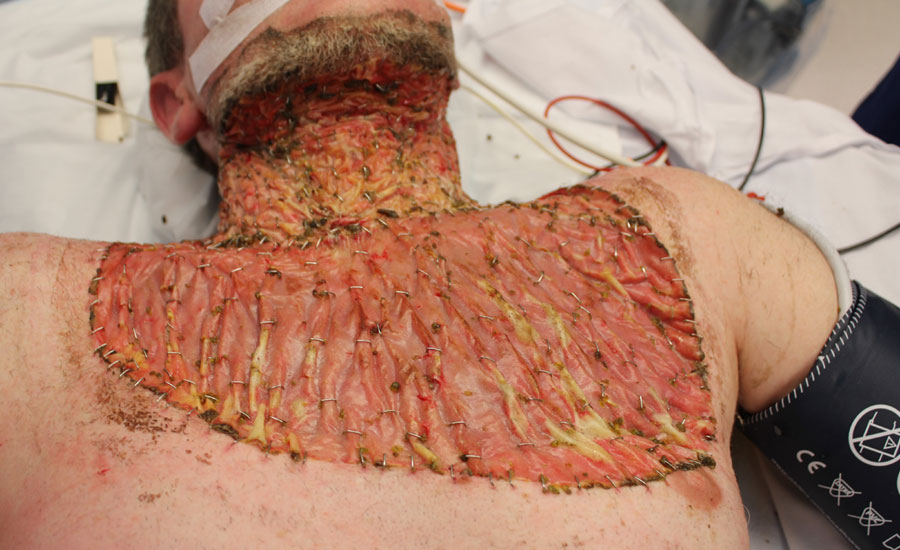
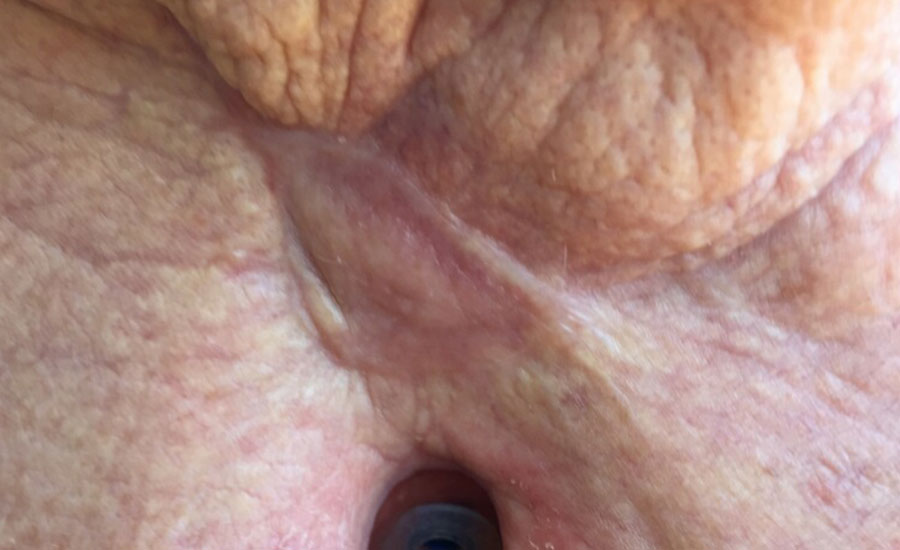
After feeling unwell with flu-like symptoms for one week, the patient presented to hospital and was diagnosed with Necrotizing Fasciitis. After debridement was performed from the bottom of chin down to chest and pre-pectoral areas, the patient was left with a large complex wound. Primary grafting was decided against due to concerns around neck contractures and restricted range of motion.
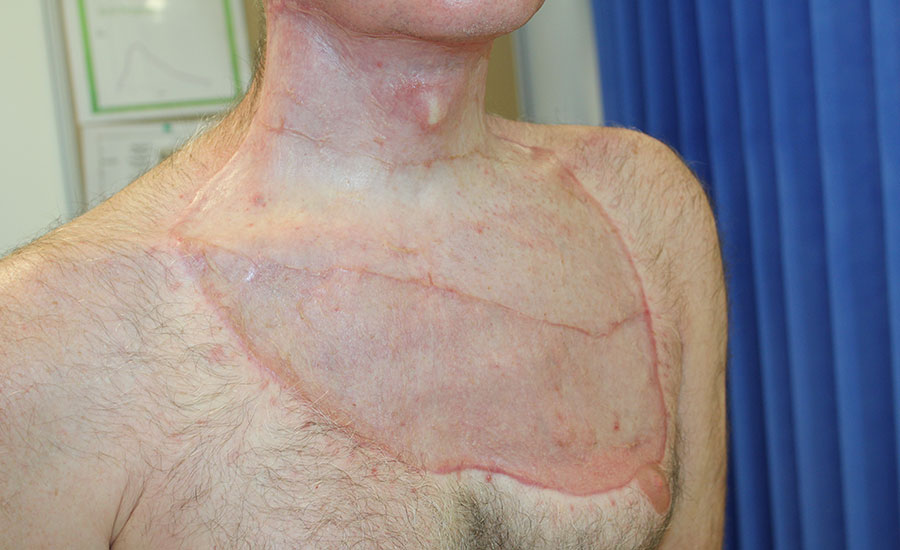
NovoSorb BTM was applied and regular dressing changes were performed twice a week. After 4 weeks BTM was delaminated and the areas grafted. The skin grafts were successful with near full range of motion and the patient resumed full-time work within three months of incident.
-
-
Chronic Wounds
-
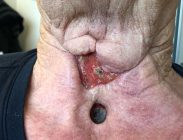
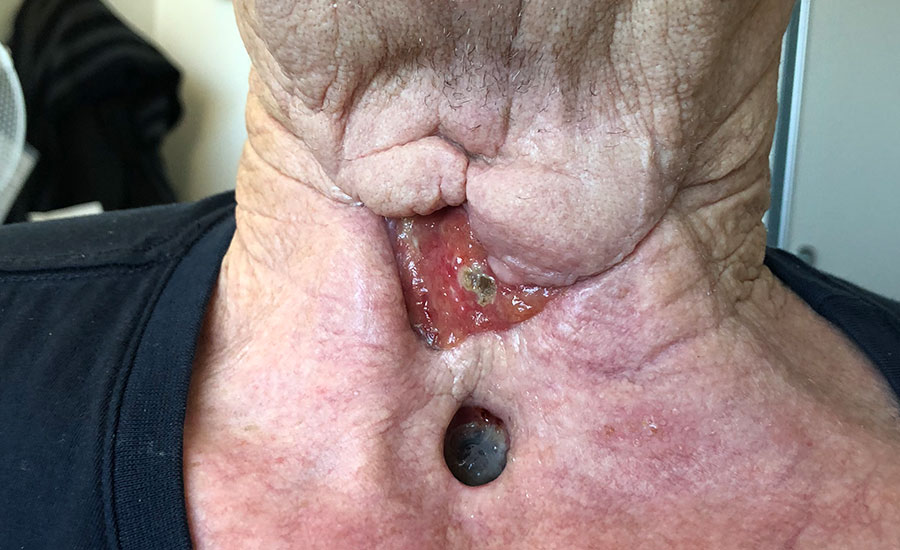
A 67 year old Caucasian male, non-smoker developed a salivary fistula after carcinoma of the vocal cord. After multiple attempts to close, there remained an open wound after 75 days. Negative Pressure Wound Therapy was not an option due to the patient having a laryngeal stoma.
After debridement NovoSorb BTM was applied with quilting staples. A silver dressing was applied and dressing changes were performed every 2-3 days to keep the area clean. At 3.5 weeks, BTM was delaminated and a split-thickness skin graft was applied, resulting in a successful closure of the wound.
-
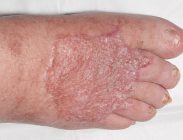
Patient developed a wound on her foot from minor trauma. Due to her diabetes and comorbidities, the wound failed to heal, developing into an infected diabetic foot ulcer (DFU). Serial debridement was performed, and she was left with a large defect on the dorsum of her foot with exposed tendons that was not suitable for skin grafting alone. NovoSorb BTM was applied, dressed and topical negative pressure wound therapy (NPWT) applied. The patient was discharged after 1 week to a care facility.
Problems with the NPWT were encountered. The patient was re-admitted with clinical evidence of infection that was systemically treated. The NovoSorb BTM was able to be retained despite the infection. Removal of the sealing membrane was performed at 4.5 weeks, a split-thickness skin graft applied, and the patient went on to heal uneventfully.
-