Whether you are a first-time user or an expert in NovoSorb® BTM (Biodegradable Temporizing Matrix) for dermal repair and reconstruction, we’re here to answer questions you may have regarding its use in a clinical setting. Below you’ll find answers to the questions we get asked the most regarding the use of NovoSorb BTM.
1. How Long Does It Take for BTM to Fully Integrate with the Wound Bed?
The time it takes for NovoSorb BTM to fully integrate varies among patients and can be influenced by several factors, including but not limited to the wound characteristics (e.g., anatomical location), patient’s age, and health status. BTM adherence to the wound bed is often evident within 2 to 3 weeks from application, with BTM’s appearance progressively changing over time as it reaches full integration. Delaminating the sealing membrane should be performed once the slowest area has integrated, which is determined by the clinician through a simple blanch test (e.g., capillary refill). Often, BTM’s appearance at full integration is described as a more uniform salmon-pink color.
As a general guideline for full integration to be achieved:
2–3 weeks – Younger, healthy patients with highly vascularized, non-mobile wounds over muscle or fascia
4–5 weeks – Elderly patients with existing comorbidities, exposed avascular structures, or highly mobile wound areas
2. Does BTM Remain in the Patient?
NovoSorb BTM’s sealing membrane is a temporary, non-biodegradable seal and will be delaminated and discarded when the surgeon deems appropriate, so long as the tissue is fully integrated throughout the BTM. Once the sealing membrane is delaminated, revealing an underlying vascularized neodermis,[1] definitive closure (e.g., skin grafting) is at the surgeon’s discretion. Given the flexibility for delamination, BTM offers surgeons the convenience to graft when ready, in stages or all at once,[2] allowing time for considerable factors such as donor site availability and patient medical concerns.
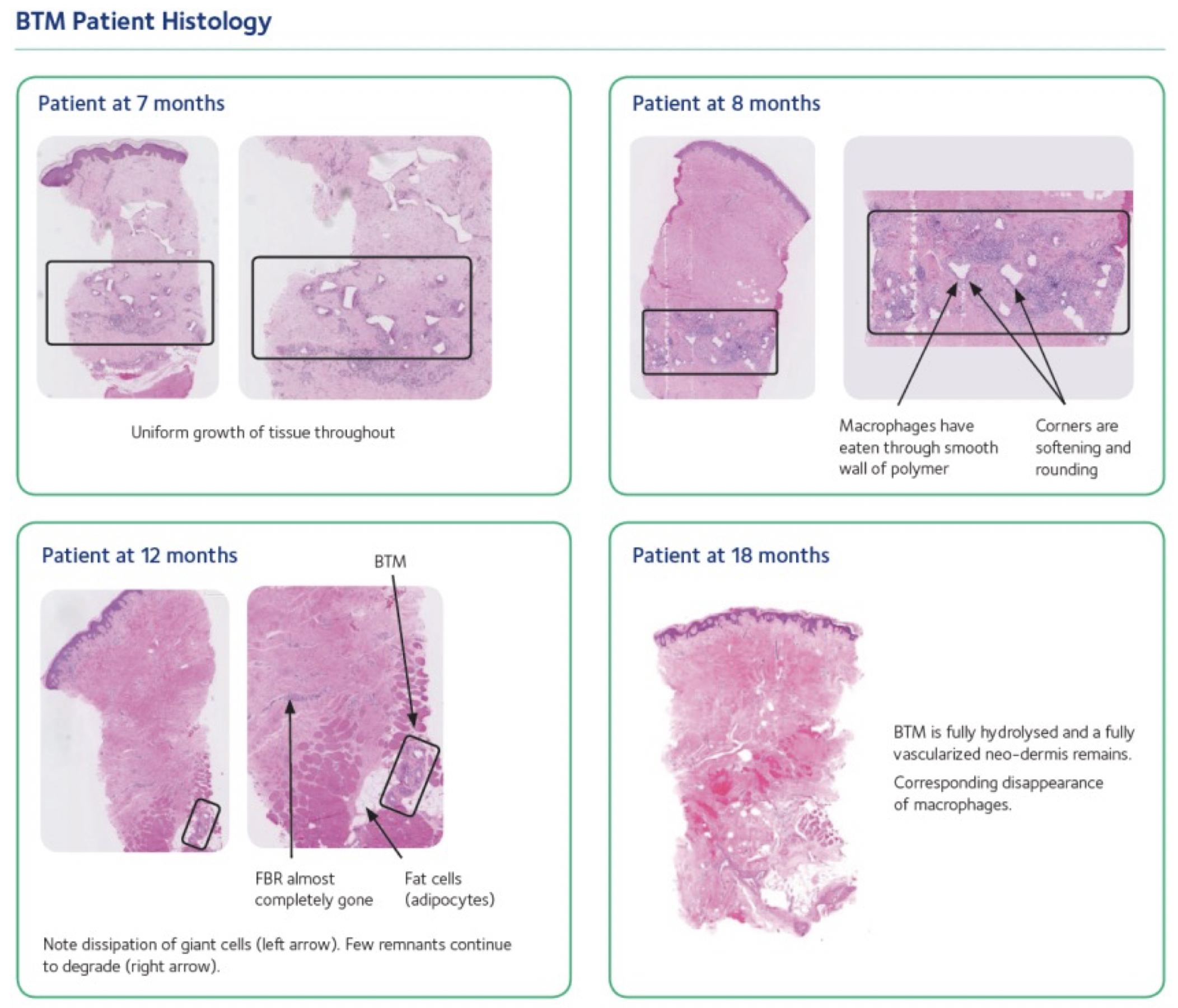
Once the sealing membrane has been removed and the surgeon has applied final closure, BTM’s biodegradable matrix remains adhered to the wound bed. The matrix is designed to remain safely in place, slowly degrading via hydrolysis, maintaining its structural integrity [1] as the body continues to heal over time. The matrix is fully resorbed and excreted in the patient’s body by 18 months.
3. How Does BTM Break Down?
NovoSorb BTM consists of medical-grade biocompatible polymers designed to facilitate tissue growth and then safely disappear as the wound continues to restructure and heal over time. BTM’s microarchitecture breaks down by infiltrating tissue, slowly degrading via hydrolysis until it fully disappears after approximately 18 months. This degradation process forms by-products such as L-lactic acid and other hydroxy acids that can be metabolized and excreted through the body’s natural pathways.
4. How Is BTM Robust in the Presence of Infection?
NovoSorb BTM is a synthetic dermal substitute made from an inert, biocompatible polyurethane material that does not contain any synthesizing proteins or act as a food source for bacteria. The use of a fully synthetic material is favorable over the use of a biological dermal substitute that provides a food source for bacteria to feed upon. [1]
BTM’s sealing membrane acts to physiologically close the wound, while the fenestrations allow for the drainage of fluid that could harbor an infection.1 BTM’s open cell matrix promotes extensive vascularization,4 allowing an infection within the matrix to be treated while BTM often remains in place. These characteristics allow for the management and treatment of localized infections without compromising BTM’s product integrity.[3]
5. Can BTM Be Applied Over Avascular Structures Such as Bone & Tendon?
Complex wounds involving deep tissue can be challenging to treat due to their lack of ample blood supply, which can heighten the risk of infection and graft failure. NovoSorb BTM is designed to integrate over avascular structures, including exposed bone and tendon,[4] if the wound bed and its margins consist of viable tissue: dermis, subcutaneous fat, muscle, paratenon, or periosteum.
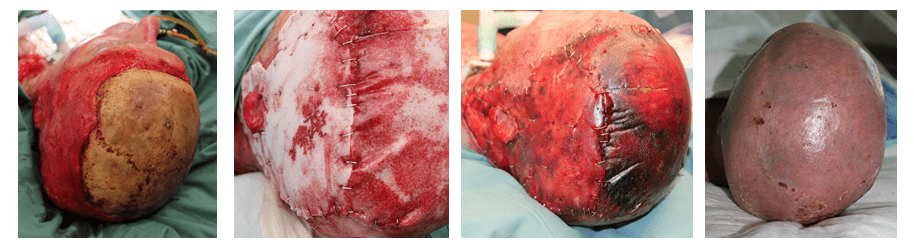
BTM may be used to bridge avascular structures such as exposed bone if they are in contact with adequate tissue surrounding the structure. BTM application over exposed bone may require the bone to be burred or drilled to induce punctate bleeding.[5] It is recommended to allow the BTM ample time to fully integrate over avascular structures, as this time is likely to increase compared to other areas.
NovoSorb BTM provides clinicians with a versatile solution that can be used to treat a variety of complex wounds. To learn more about how BTM is designed to minimize scarring and contracture for improved functional and cosmetic outcomes, [3] contact one of our knowledgeable team members at (302) 268-6163.
Note: this document contains general guidelines and is not designed to replace existing institutional protocols or professional clinical judgment regarding patient care. Please refer to the instructions for use.
______________
[1] Wagstaff MJD, Schmitt B, Caplash Y, Greenwood JE. Free flap donor site reconstruction: A prospective case series using an optimized polyurethane temporizing matrix. Eplasty. 2015; 15:231–48.
[2] Greenwood JE, Schmitt BJ, Wagstaff MJD. Experience with a synthetic bilayer Biodegradable Temporizing Matrix in significant burn injury. Burns Open. 2018;2(1):17-34.
[3] Solanki NS, York B, Gao Y, Baker P, Wong She RB. A consecutive case series of defects reconstructed using NovoSorb® Biodegradable Temporising Matrix: Initial experience and early results. Journal of Plastic, Reconstructive & Aesthetic Surgery. 2020; 73(10):1845–53.
[4] Damkat-Thomas L, Greenwood JE, Wagstaff MJD. A synthetic Biodegradable Temporizing Matrix in degloving lower extremity trauma reconstruction: A case report. PRS Global Open; 2019; 7(4):e2110.
[5] Jennings M, Willet J, Coghlan P, Solanki NS, Greenwood JE. Biodegradable temporising matrix in severe meningococcal septicaemia: A case report. Australasian Journal of Plastic Surgery. 2021; 4(1):67–70.


