Case Report
Hospital MetroHealth Medical Center, Cleveland, OH
Finger wound with exposed bone required an alternative reconstruction solution after a failed graft.
The patient sustained a self-inflicted gunshot wound to the ring finger resulting in a middle phalanx fracture and a dorsal soft-tissue defect. Initial soft-tissue reconstruction with a full-thickness skin graft over the fracture and extensor tendon repair was unsuccessful. To avoid further donor site morbidity and to maximize functionality, NovoSorb® BTM was chosen to salvage the finger over more complex local flap options. NovoSorb BTM successfully integrated over the exposed bone, which was devoid of periosteum. After the NovoSorb BTM sealing membrane was removed, the wound bed was left to re-epithelialize, eliminating the requirement for a skin graft.
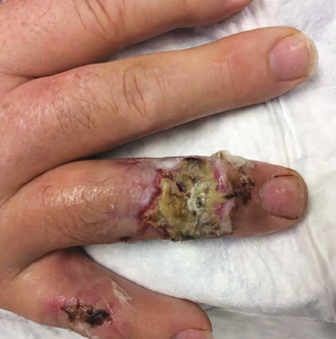
Figure 1: Soft-tissue infection of the dorsal digitus medicinalis after initial reconstructive attempt with full thickness skin graf.
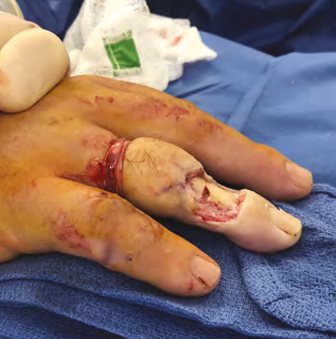
Figure 2: Post debridement removing non-viable skin graft, skin, and extensor tendon repair.

Figure 3: 9 days post NovoSorb BTM application: early revascularization is evident without signs of infection or fluid collection.

Figure 4: 6 weeks post-operative: NovoSorb BTM delaminated with notable healthy granulation tissue.

Figure 5: 7 weeks post-delamination: wound closure via re epithelialization without requiring a skin graft.

Figure 6: 275 days post-operative: stable mature scar, with pliable skin and minimal contractures.
Background
Treatment
Outcome
A 68-year-old male, with no significant medical history, sustained a self-inflicted gunshot wound to the ring finger of the right hand, resulting in an unstable middle phalanx fracture and dorsal soft tissue loss with zone 2 extensor tendon injury. The patient underwent immediate debridement with K-wire pinning of the fracture, primary repair of the extensor tendon, and full-thickness skin graft for soft tissue reconstruction and coverage. Further reconstruction to salvage the finger was required after infection and failure of the skin graft (Fig 1).
Reconstructive options included a reverse cross-finger flap with a skin graft or finger amputation. The local flap was discussed and ultimately rejected as it required the use of an uninjured finger as the donor site. Both surgeon and patient had concerns about post-operative stiffness and loss of motion. Amputation was also rejected by the patient. NovoSorb BTM was selected as the most suitable reconstructive option to limit donor site morbidity, allowing prompt patient discharge and early occupational therapy.
The non-viable skin graft, skin, and failed extensor tendon repair were debrided to healthy bleeding tissue which led to a 1.5×1.5 cm skin defect with an exposed middle phalanx devoid of periosteum (Fig 2). The unstable middle phalanx fracture and distal interphalangeal (DIP) joint were stabilized with a 0.062 K-wire driven retrograde across the joint and fracture. The extensor tendon had a 2 cm defect after debridement and was not reconstructed. Two unicortical holes were created in the middle phalanx to stimulate bleeding to help with vascularization of the dermal template.
NovoSorb BTM was trimmed to fit the defect and secured with a running chromic suture. A bolster dressing was applied and the patient was discharged on oral antibiotics. At nine days postapplication of NovoSorb BTM, the bolster surgical dressing was removed. Early revascularization was evident without any signs of infection or underlying fluid collection (Fig 3). The patient was referred to occupational therapy for splint fabrication to stabilize the DIP joint and start an active range of motion at the proximal interphalangeal (PIP) joint. Local wound care consisted of a nonadherent gauze dressing and a compressive wrap. The patient was seen periodically and, at six-weeks post-operatively, the NovoSorb BTM sealing membrane was delaminated revealing healthy granulation tissue on the wound base (Fig 4).
At 7 weeks post-delamination, the wound base re-epithelialized (Fig 5), and one month later (77 days post NovoSorb BTM application) the skin continued to mature and become more pliable and stable (Fig 6). Both the patient and surgeon were satisfied with the spontaneous re-epithelialization, eliminating the need for a skin graft. The patient recovered a full active PIP joint range of motion and had a stable arthrodesis of the DIP joint that allowed for use of the hand for activities of daily living. The soft-tissue reconstruction of the dorsal finger defect was successful through the incorporation of NovoSorb BTM in a single surgery to salvage the finger, despite the exposed bone and lack of periosteum, without the need for more complex reconstructive options.




