Case Report
Hospital Middlemore Hospital, New Zealand
Trauma to the blood vessels limited flap surgery as a viable option, so NovoSorb® BTM was used for soft tissue reconstruction to provide coverage for the exposed structures.
Healthy male sustained partial right-hand amputation and degloving of forearm, with exposed tendons, due to a motor vehicle accident. The wound was not suitable for immediate skin grafting due to the exposed tendons and the need for deferred tendon reconstruction. A free flap was considered but excluded due to concerns around using previously traumatized donor vessels for microvascular anastomosis.

Figure 1: Initial presentation of injury.
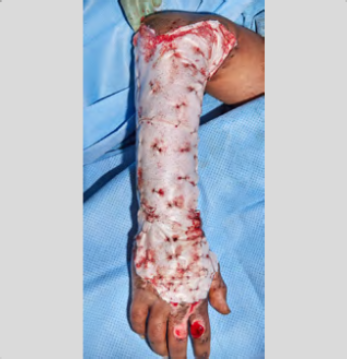
Figure 2: Application of NovoSorb BTM.

Figure 3: Day 19 after NovoSorb BTM application; matrix appears well vascularized and integrated.

Figure 4: Day 28 after NovoSorb BTM application; sealing membrane delaminated and neodermis refreshed with dermabrasion.

Figure 5: 6 months post skin grafting.

Figure 6: 11 months post skin grafting; reconstruction of EPL tendon restoring function to the hand.
Background
Treatment
Outcome
A 28-year-old Indian male was involved in a high-speed motor vehicle accident on a motorway. During the crash, his right hand was raised to shield his face, resulting in his hand piercing the windshield. The patient sustained a partial amputation of his right hand with fracture of the distal radius, ischemia of the hand with injury to the radial and ulnar arteries, laceration of several tendons, and degloving of the right forearm soft tissues (Fig. 1). The patient had no significant comorbidities.
Initial treatment was provided at Auckland Hospital, where the fracture was reduced with K-wires, radial and ulnar arteries were repaired, arterial inflow to the hand was restored, and the non-viable skin was debrided. The wound was initially managed using negative pressure wound therapy (NPWT).
The patient was transferred to Middlemore Hospital, where he underwent further debridement and application of NPWT until the remaining skin appeared viable. The wound was not suitable for immediate skin grafting due to the exposed tendons and the need for deferred tendon reconstruction. A free flap was considered but excluded due to concerns around using previously traumatized donor vessels for microvascular anastomosis.
After the second debridement, NovoSorb BTM was applied to the wound bed and held in place with staples on the wound margin and quilting staples across the surface (Fig. 2). Initial outer dressings consisted of an antimicrobial silver dressing and NPWT. NovoSorb BTM application was reviewed at 1 week, with dressings changed on the ward. NovoSorb BTM was subsequently dressed with an antimicrobial silver dressing and bandage, with changes occurring twice a week. After 19 days, NovoSorb BTM appeared vascularized and integrated (Fig. 3). At 4 weeks post NovoSorb BTM application, the sealing membrane was delaminated, the neodermis was lightly refreshed using dermabrasion, and a split-thickness skin graft was applied and dressed (Fig. 4).
5 days post skin grafting, the outer dressing was removed to show complete take of the skin graft. Following graft take, occupational therapy commenced and the skin graft matured with a good esthetic and functional result. At 6 months post grafting, a tendon transfer was performed to reconstruct the damaged EPL tendon, restoring function to the patient’s hand (Fig. 5 and 6).




